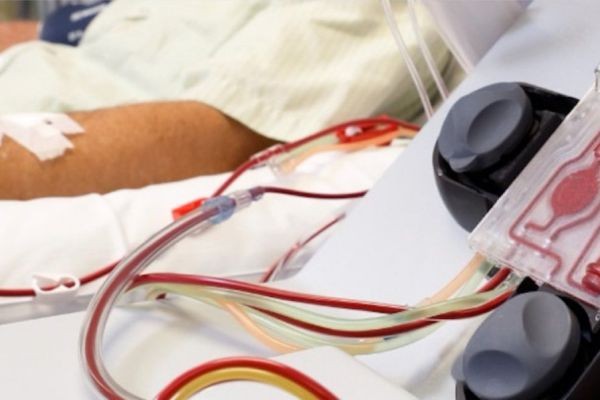
Hospitals are quietly rewriting how complex blood disorders are managed as pressure on advanced therapies increases. Inside this shift, strategic leaders are increasingly evaluating the apheresis market long-term outlook as a framework for planning infrastructure, clinical capabilities, and patient access pathways.
What was once considered a niche intervention is now entering boardroom discussions where cost efficiency and treatment precision intersect. The apheresis market long-term outlook is being shaped not only by clinical demand but also by how healthcare systems adapt to high complexity procedures that require specialized equipment and trained teams.
Therapeutic Apheresis Procedure For Autoimmune Diseases And Clinical Relevance In Market Evolution
Inside a busy hospital strategy room, therapeutic decisions are rarely isolated from financial and operational realities. One of the most closely examined areas is the therapeutic apheresis procedure for autoimmune diseases, which is increasingly used when conventional treatments fail to deliver stable outcomes. This procedure enables selective removal of harmful components from blood, offering clinicians a targeted way to manage conditions that are otherwise difficult to control.
The rising attention toward therapeutic apheresis treatment applications is tied to growing recognition of immune mediated disorders and chronic inflammatory conditions. Hospitals are now weighing how early intervention using apheresis can reduce long term complications and repeated admissions. This shift is influencing procurement decisions, training requirements, and investment in specialized clinical units.
From a market perspective, the apheresis ecosystem is responding to demand for precision based interventions. The expansion of indications beyond rare diseases into more common autoimmune and neurological conditions is reinforcing its relevance. At the same time, clinical leaders are evaluating how integration of apheresis can reduce dependency on long duration pharmacological therapies, which often carry systemic side effects.
The broader implication is clear. As clinical utility expands, decision makers are no longer viewing apheresis as an isolated treatment but as part of a comprehensive care model. This transformation is steadily reinforcing confidence in the apheresis market long-term outlook across both developed and emerging healthcare systems.
Apheresis Types Used In Clinical Practice And Their Role In Treatment Pathways
Different clinical scenarios demand different approaches, which is why understanding apheresis types used in clinical practice has become essential for hospital planning teams. From plasma exchange to leukapheresis and platelet removal techniques, each method serves a distinct therapeutic purpose and requires tailored infrastructure.
These variations influence not only treatment outcomes but also operational planning. Facilities that handle high patient volumes often invest in flexible systems capable of switching between multiple procedures. This adaptability is becoming a defining factor in procurement decisions, especially in tertiary care centers where case diversity is high.
The blood apheresis procedure benefits extend beyond immediate clinical results. Reduced symptom severity, faster stabilization in critical conditions, and lower recurrence rates are increasingly documented advantages that support its adoption. These outcomes are particularly relevant in intensive care environments where time sensitive interventions are critical.
As hospitals refine their service lines, they are also considering workforce specialization. Nurses and technicians trained in apheresis procedures are becoming key assets in delivering consistent care quality. This has led to structured training programs and partnerships with device manufacturers to ensure procedural accuracy and safety.
The combination of clinical effectiveness and operational complexity is reshaping how healthcare providers assess investment priorities. In this context, the apheresis market growth drivers are increasingly linked to both technological advancement and institutional readiness to adopt advanced therapeutic systems.
Beyond clinical walls, policy and reimbursement frameworks are also influencing adoption rates. Systems that recognize the long term cost benefits of apheresis over repeated conventional therapies are creating stronger incentives for adoption. This alignment between clinical value and financial logic is reinforcing sustained interest in the sector.
As these dynamics converge, healthcare leaders are beginning to view apheresis not as a supplementary option but as a strategic capability. This shift is expected to continue influencing infrastructure planning and treatment protocols in the years ahead.
The long term trajectory of the field reflects a broader transformation in medicine itself, where precision and adaptability define value. As clinical demand expands and institutional readiness improves, the ecosystem surrounding apheresis is likely to mature into a more integrated and essential component of modern care delivery. The evolving patterns suggest a future where strategic planning and clinical innovation move in closer alignment than ever before.